Table of Contents
- How Car Accidents Cause Serious Injuries: Crash Forces, Hidden Trauma, and Legal Implications
- The Physics Behind Injury
- The Kinematics of Trauma: The Three Collisions
- Collision Phases and Injury Patterns
- Cervical Spine Trauma and Whiplash Pathology
- Conclusion: Act Early, Diagnose Precisely
- FAQ: Car Accident Injuries
Motor vehicle collisions expose the human body to powerful forces capable of causing serious trauma. When injuries occur, victims often require both medical treatment and reliable legal support. A careful review of the circumstances, liability, and resulting damages can play an important role in recovering compensation for the harm caused by negligent drivers.
Severe collisions frequently lead injured individuals to seek legal support from someone who understands how accident injuries develop and how to prove the connection between the crash and the resulting medical conditions.
When injuries disrupt daily life, experienced legal help can ensure that medical evidence, accident reports, and witness testimony are properly preserved. Legal guidance from a Texas personal injury lawyer becomes particularly important when insurers dispute the severity of injuries or attempt to minimize financial responsibility.
How Car Accidents Cause Serious Injuries: Crash Forces, Hidden Trauma, and Legal Implications
Car accidents produce rapid, high-energy transfers that disrupt tissue at both macroscopic and microscopic levels. These collisions do not simply cause pain. They initiate a cascade of mechanical deformation, cellular injury, and delayed inflammation that can evolve over hours or days. The sudden deceleration forces involved in a crash place stress on muscles, ligaments, nerves, and internal organs, which leads to both immediate and delayed symptoms.
Collisions involving commercial vehicles generate significantly greater momentum. In those cases, a San Antonio truck accident lawyer may investigate driver fatigue, vehicle maintenance failures, and federal transportation safety violations.
Many acute injuries from a car accident remain invisible in the early stages. Soft tissue damage, concussions, and internal bleeding often develop without obvious external signs. As inflammation increases, patients may begin to experience neck pain, back stiffness, headaches, or neurological symptoms. This delayed presentation explains why individuals often feel “fine” immediately after a crash but worsen within 24 to 72 hours.
Complex injury claims frequently involve teams of personal injury attorneys who work with physicians and biomechanical experts to demonstrate how the crash produced specific injuries.
To properly evaluate acute injuries from a car accident, you must connect physics, anatomy, and clinical presentation. Understanding how force transfers through the body helps identify injury patterns, guide diagnostic testing, and prevent minor trauma from progressing into chronic pain or long-term disability.
The Physics Behind Injury
Crashes often require a specialized investigation because these collisions can involve complex regulatory and liability considerations.
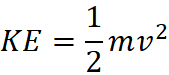
Velocity drives injury severity in any motor vehicle collision. As speed increases, the energy transferred into the body rises exponentially. Even a modest increase in speed can dramatically increase the force applied to muscles, bones, and internal organs during impact.
Legal teams often rely on this physical relationship when explaining why high-speed collisions frequently cause severe trauma even when vehicle damage appears limited.
When a crash occurs, the body undergoes rapid deceleration. Tissues absorb force at different rates. Dense structures such as bone resist motion, while softer tissues—like the brain, liver, and muscles—deform under stress. This difference creates shear forces, which are the primary mechanism behind many acute car accident injuries, including concussions, internal bleeding, and ligament damage.
Establishing how these forces caused injury is often central to an accident claim because insurers frequently dispute causation.
These biomechanical forces also explain why internal injuries after a car accident often occur without obvious external trauma. Energy travels through the body, not just across the surface, which places internal organs and neurological structures at significant risk.
In cases involving severe trauma, a car accident lawyer in San Antonio may present expert testimony explaining these biomechanical injury mechanisms.
Clinical implication: high-speed collisions significantly increase the likelihood of serious injury, even when vehicle damage appears minor.
The Kinematics of Trauma: The Three Collisions
Understanding the sequence of collisions allows clinicians and attorneys to predict injury patterns with precision. Every crash unfolds in three distinct phases, and each phase produces specific acute injuries from a car accident.
Complex crash cases often involve collaboration between physicians, engineers, and a traffic accident lawyer who evaluates liability and damages.
1. Vehicular Collision
Energy transfers through the vehicle frame at the moment of impact. Structural integrity—such as crumple zones—determines how much force reaches the passenger compartment. Higher speeds and direct impacts increase force transmission and injury risk.
Injury claims arising from this phase frequently require analysis from a lawyer who understands how vehicle damage reflects the magnitude of force involved.
2. Body Collision
The occupant decelerates abruptly and contacts the steering wheel, dashboard, seatbelt, or airbag. Even with proper restraint, the body experiences intense compressive and rotational forces. These forces commonly cause whiplash injuries, joint trauma, and soft tissue damage.
Medical documentation of these injuries often becomes critical evidence in cases handled by an auto injury attorney.
3. Organ Collision
Internal organs continue moving after the body stops. This phase produces some of the most serious and least visible injuries.
- Brain movement within the skull
- Liver and spleen compression
- Lung contusions
Key insight: many internal injuries after a car accident originate during this phase, not at the moment of vehicle impact.
Severe internal trauma frequently becomes the focus of litigation handled by a PI attorney because these injuries often require extensive medical treatment.
Collision Phases and Injury Patterns
| Collision Phase | What Happens | Common Injuries | Clinical Significance |
| Vehicular Collision | Vehicle absorbs and transfers energy | Structural intrusion, blunt force trauma | Determines force magnitude entering cabin |
| Body Collision | Occupant strikes interior/restraints | Whiplash, fractures, joint injuries | Primary source of musculoskeletal injury |
| Organ Collision | Internal organs continue moving | Concussion, internal bleeding, contusions | Often invisible; high risk if untreated |
Clinical takeaway: each phase builds on the previous one. By the time organ collision occurs, energy has already transferred through the vehicle and body, which amplifies the risk of hidden and delayed injuries.
Neurological Trauma: The Invisible Injury
Brain injuries caused by car accidents often present without immediate radiographic findings. Clinical suspicion must guide early intervention.
Coup-Contrecoup Dynamics
Dual-impact injury leads to localized bruising and diffuse swelling. Patients may initially appear stable but deteriorate as edema develops.
Diffuse Axonal Injury (DAI)
Rotational acceleration disrupts neuronal connections. This injury affects brain signaling rather than structure.
Common symptoms include:
- Slowed cognition
- Difficulty concentrating
- Behavioral changes
Intracranial Hemorrhage
Bleeding increases intracranial pressure and reduces cerebral perfusion. Without intervention, this leads to herniation.
Insight: even mild traumatic brain injury symptoms after a car accident can signal deeper pathology. Early neurological assessment remains essential.
Cervical Spine Trauma and Whiplash Pathology
Whiplash represents a complex biomechanical injury rather than a simple muscle strain.
The S-Curve Mechanism
The cervical spine briefly forms opposing curves under acceleration. This abnormal motion stresses ligaments, discs, and joints simultaneously.
Additional Clinical Considerations
- Muscle microtears: contribute to delayed stiffness
- Proprioceptive disruption: affects balance and coordination
- Chronic pain pathways: develop when acute injury goes untreated
Long-Term Risk
Untreated cervical injuries can progress to:
- Chronic neck pain
- Reduced range of motion
- Persistent headaches
Seatbelt Syndrome and Internal Injuries
Seatbelts redistribute force across the torso. This protection comes with predictable injury patterns.
The Seatbelt Sign as a Diagnostic Tool
Visible bruising correlates with deeper trauma. Physicians treat this as an indicator for advanced imaging.
Expanded Internal Injury Risks
- Mesenteric tears: disrupt blood supply to the intestines
- Liver lacerations: lead to internal hemorrhage
- Diaphragmatic rupture: allows abdominal organs to shift into the chest cavity
Vascular Trauma
Deceleration can stretch and tear major vessels. These injuries often present with minimal early symptoms but carry high mortality.
Key point: symptoms of internal bleeding after a car accident may remain subtle until the condition becomes critical.
Orthopedic and Extremity Trauma
Orthopedic injuries often define functional recovery and long-term disability.
Lower Extremity Load Transmission
Force entering through the knees travels upward into the pelvis and spine. This kinetic chain explains multi-level injuries.
Upper Extremity Reflex Response
Drivers instinctively brace for impact. This reaction increases risk of:
- Wrist fractures
- Elbow injuries
- Shoulder dislocations
Soft Tissue Damage
Ligaments and tendons fail under tension before bone fractures occur in some cases. These injuries often require advanced imaging to diagnose.
Delayed Symptoms and the Physiological Mask
The body prioritizes survival during trauma. Pain signals do not always reflect injury severity.
Neurochemical Suppression
Adrenaline and endorphins reduce pain perception immediately after impact.
Inflammatory Cascade
Tissue damage triggers swelling, which develops over time. This process explains:
- Delayed neck stiffness
- Increasing back pain
- Late-onset headaches
Clinical Risk
Patients who delay evaluation often present with worsened conditions that require more intensive treatment.
Key takeaway: delayed pain after a crash often signals evolving injury, not minor trauma.
Read our article, What to Do After a Car Accident That Is Not Your Fault, to learn what steps can help protect your health and your claim after a crash.
Diagnostic Strategy: A Layered Approach
Accurate diagnosis requires matching imaging modality to suspected injury.
Advanced Considerations
- CT scans identify life-threatening bleeding quickly
- MRI detects soft tissue disruption with high sensitivity
- DTI reveals microscopic brain injury not visible on standard imaging
Functional Testing
Electrodiagnostic studies assess nerve damage when patients report:
- Tingling
- Weakness
- Radiating pain
Conclusion: Act Early, Diagnose Precisely
Car accidents in Texas generate forces that disrupt the body at every level. The absence of immediate symptoms does not indicate safety. Many of the most serious conditions—brain injury, internal bleeding, and ligament damage—develop over time.
Early medical evaluareas-sation, targeted imaging, and structured follow-up care define recovery outcomes.
Legal guidance from an experienced Texas car accident injury lawyer often becomes essential when victims must prove that a negligent driver caused these injuries.
Bottom line: treat every collision as a medical event, not just an inconvenience.
FAQ: Car Accident Injuries
How do I know if I have a serious injury after a car accident?
A serious injury after a car accident can exist without severe pain. Warning signs include headache, dizziness, confusion, numbness, and abdominal pain. These symptoms often indicate acute car accident injuries such as concussion, whiplash, or internal bleeding. Seek medical evaluation within 24–72 hours.
What injuries are most commonly missed after a car accident?
The most commonly missed injuries after a car accident include concussions, ligament damage, disc herniations, internal bleeding, and nerve compression. These hidden injuries after a car accident often worsen over time and may not appear on initial imaging.
Why does my neck hurt a day after a car accident?
Neck pain after a car accident often results from whiplash injury. The cervical spine stretches beyond normal limits during impact. Inflammation develops over 24–48 hours, which causes delayed stiffness and pain.
Can internal injuries occur without visible bruising after a crash?
Internal injuries after a car accident can occur without visible bruising. Organs continue moving after impact, which can cause bleeding or tearing. Symptoms such as dizziness, weakness, or abdominal pain may appear hours later and require immediate evaluation.
What does a headache after a car accident usually mean?
A headache after a car accident may indicate a concussion, neck strain, or intracranial bleeding. Persistent or worsening headaches are a key sign of traumatic brain injury symptoms and require prompt medical evaluation.
How long after a car accident should I see a doctor?
You should see a doctor within 24–72 hours after a car accident. This timeframe allows early detection of delayed injuries and helps establish a clear medical connection between the accident and your symptoms.
Can a low-speed car accident cause real injuries?
A low-speed car accident can still cause real injuries, including whiplash, concussions, and soft tissue damage. Injury risk increases if the body is unprepared or the head is turned at impact.
What are signs of nerve damage after a car accident?
Signs of nerve damage after a car accident include tingling, burning pain, weakness, and radiating pain into the arms or legs. These symptoms often indicate nerve compression or spinal injury.
What should I do if pain gets worse after a car accident?
Worsening pain after a car accident often signals inflammation or structural injury. Seek medical evaluation if pain increases, spreads, or limits movement. Early treatment reduces the risk of chronic pain.
How do doctors diagnose hidden injuries after a car accident?
Doctors diagnose hidden injuries after a car accident using CT scans for internal bleeding, MRI for soft tissue damage, neurological exams for brain injury, and EMG testing for nerve damage. Early testing helps confirm injuries before symptoms worsen.
